Thyroid cancer cases are rising across the globe—but why? Is it simply better detection, or are lifestyle and environmental factors silently driving this surge? Could obesity, radiation, or even everyday chemicals be putting millions at risk?
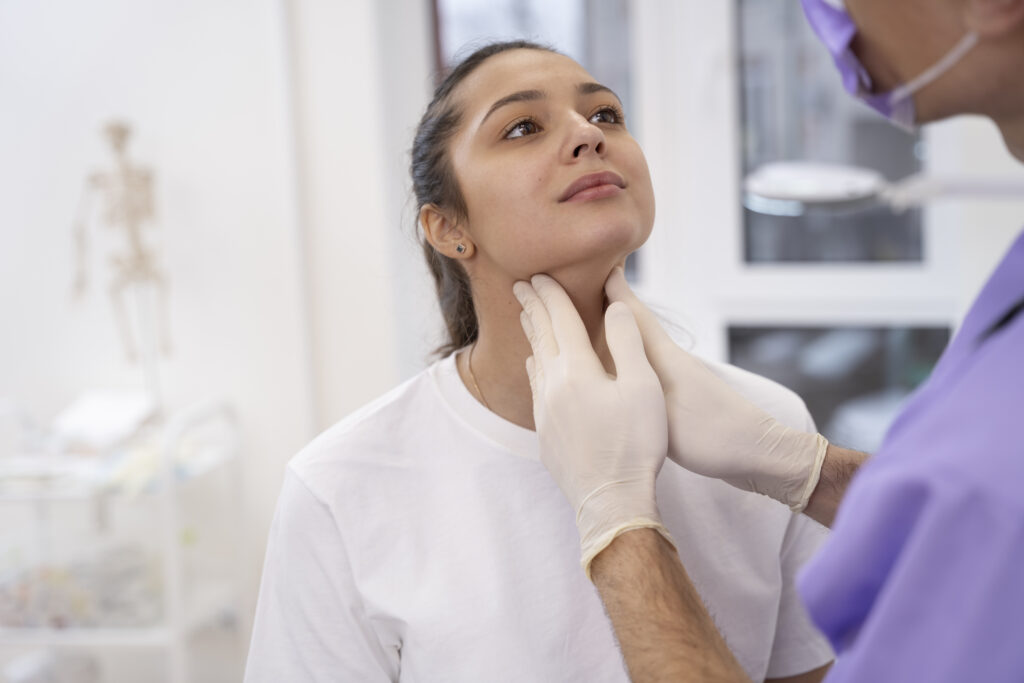
Thyroid cancer, affecting the small butterfly-shaped gland at the base of the neck, is increasing faster than most other cancers in many countries. The thyroid regulates metabolism, heart rate, body temperature, and weight. Cancer develops when its cells grow uncontrollably, forming tumors that can sometimes spread to nearby tissues or other organs. While most cases are treatable, the rapid rise in diagnoses has experts concerned.
In the United States, SEER data shows that between 1980 and 2016, thyroid cancer cases more than tripled—from 2.39 to 7.54 per 100,000 men, and 6.15 to 21.28 per 100,000 women. “Thyroid cancer is one of the few cancers still on the rise despite medical advances,” says Sanziana Roman, endocrine surgeon at UCSF.
Radiation exposure in childhood is a known risk factor. Events like the Chernobyl disaster caused spikes in children, and atomic-bomb survivors in Japan showed similar trends. Yet in countries like the US, without such nuclear exposure, the rise puzzled experts.
Part of the explanation lies in improved detection. The introduction of thyroid ultrasonography in the 1980s and fine-needle biopsies in the 1990s allowed doctors to identify very small tumors that previously went unnoticed. “We can now detect tiny papillary cancers that are often slow-growing and harmless,” explains epidemiologist Cari Kitahara. Overdiagnosis is evident in countries like South Korea, where thyroid cancer rates soared after nationwide screening programs and dropped when the programs were reduced.
Detection alone, however, does not explain the full picture. Middle-income countries without extensive screening are also seeing increases, and larger, more aggressive tumors are being diagnosed more frequently. Obesity has emerged as a key factor, with high BMI linked to both higher risk and more aggressive disease. Hormonal imbalances, especially elevated thyroid-stimulating hormone (TSH), may further contribute.
Environmental exposures are also under investigation. Endocrine-disrupting chemicals in household products, trace elements in volcanic regions, and medical radiation from CT scans may all play a role. “It’s likely a multifactorial phenomenon,” says Roman. “Lifestyle, environmental, dietary, hormonal, and genetic factors interact to influence thyroid cancer risk.”
Treatment has improved, with partial thyroid removal and targeted radioactive iodine use now common, reducing unnecessary complications. Yet the rising incidence raises urgent questions. Thyroid cancer is usually treatable, but understanding why it is increasing globally is crucial. Are we seeing a hidden epidemic, or is modern medicine simply uncovering a problem that has always existed?
















Downloaded the 661betapp. Navigation is smooth and the odds seem pretty competitive. A solid option for mobile betting addicts like myself. Grab the app 661betapp.
Sol Casino bietet ein umfangreiches Angebot
an Spielen, darunter Slots, Tischspiele, Live Casino und Crash Games.
Wir bieten Ihnen ein umfangreiches Portfolio
an Spielen, von Slots bis hin zu Live-Tischspielen, sowie innovative Zahlungsmethoden und professionelles Kundenservice.
Mit über 7.000 Slot-Maschinen, Live-Tischspielen und einer
Vielzahl an anderen spannenden Spielen findest du sicherlich
das Richtige für dich. Neue Spieler erhalten bis zu 500 € Bonus plus 200 Freispiele.
Das bedeutet, dass das Casino sich an strenge Richtlinien und Sicherheitsstandards halten muss, um sicherzustellen, dass Spieler in einem fairen und sicheren Umfeld spielen können.
Die Casino-Branche setzt sich ständig fort, und Sol Casino ist da, um Ihnen zu
helfen, Ihren Traum von Glücksspielen zu verwirklichen! Um den Bonus freizuspielen, müssen Spieler mindestens 40-fach das Bonusbetrag einspielen. Sol Casino bietet eine umfangreiche Auswahl an Spielen, darunter Slots,
Tischspiele, Live-Casino-Spiele und viele mehr.
Mit unserer riesigen Auswahl an 7.000 Slots, den beliebtesten Tischspielen und Live-Casino-Aktionen garantieren wir Ihnen unvergleichliche Unterhaltung und spannende Spieleerfahrungen.
Die mobilen Version von Sol Casino ist ideal für Spieler, die unterwegs spielen möchten und trotzdem eine
umfassende Erfahrung benötigen.
References:
https://online-spielhallen.de/smokace-login-dein-tor-zum-spielvergnugen/
About to Dive into pk36game! Wish me luck. Maybe this will become my new favorite? Take a look here: pk36game
Support can be contacted via email or live
chat, so you can pick the method that works best for you.
The team is made up of skilled and experienced professionals who are ready to help you every step of the way.
The Lucky Green support team is available around the clock to assist with any questions or issues you might
have. With secure and flexible options, withdrawing your winnings
is simple and hassle-free. If you have any questions or need
updates on your transaction, the customer support team is ready to assist.
The platform accepts AUD without conversion fees, saving
you money on every transaction. Regular security updates keep the platform protected against emerging threats.
Two-factor authentication adds an extra security layer to your account.
The casino utilizes advanced 256-bit SSL encryption (the same technology banks use) to safeguard
your personal and financial data. Lucky Green operates under a
Curacao eGaming license, ensuring regulatory compliance and player protection. E-wallet withdrawals take slightly longer at 6-12 hours, while bank transfers typically arrive within 24 hours.
References:
https://blackcoin.co/playamo-casino-safe-online-casino-in-australia/
Zoome Casino is a leader in the Australian online gaming market because it always tries to innovate and provide
a high-quality experience. Whether you're a beginner or an experienced player, Zoome
Casino has something to offer. The platform runs smoothly
on both iOS and Android devices, providing access to all essential features,
including games, payments, and customer service.
Advanced SSL encryption technology protects user data and transactions, providing a safe environment for all players.
A license means the platform is held to fair play and financial standards.🔐 Strong securityLook for SSL encryption, secure payment methods,
and clear privacy policies. When it comes to online gambling, safety and trust should always come first
– and Zoome Casino absolutely delivers.
You can start playing today with a generous welcome bonus and enjoy non-stop entertainment wherever you are
in Australia. Just open your browser, log in, and you’re ready to play — it’s
that simple.Wherever you are in Australia, your casino is
right there with you. Whether you’re on a lunch break, relaxing at
home, or out and about, Zoome runs smoothly on any mobile browser — no
downloads required.The site is fully optimised for both Android and iOS devices, meaning
it automatically adjusts to your screen for a fast,
clean and responsive experience. Safe, fast, and 100%
player-focused — it’s no wonder more Australians are joining every day.🎉 Ready to jump
in?
You can always check the RTP in the Zoome casino info panel of
each game before you play. These allow players to control how much they spend over a daily, weekly, or monthly period.
Self-exclusion tools are available for players who
feel the need to take a break. Zoome Casino recommends that players avoid using shared passwords and change
login credentials regularly. The platform uses 256-bit SSL encryption to
secure all transactions, including deposits, withdrawals, and login sessions.
References:
https://blackcoin.co/top-online-casinos-and-games-in-new-zealand/
online casino uk paypal
References:
https://empleos.getcompany.co/
mobile casino paypal
References:
arlogjobs.org
casino mit paypal einzahlung
References:
robbarnettmedia.com
online casino mit paypal
References:
jobspaceindia.com
Chơi slots nhận thưởng chỉ với 3 biểu tượng trở lên. 3D slots, video slots, megaway slots, jackpot lũy tiến,… tất cả các dòng game quay hũ kinh điển nhất hiện nay đều có tại xn88 . Chúng tôi mang đến cho hội viên hơn 1.000+ vòng quay miễn phí với mức RTP cực cao. TONY03-09
Hơn 1.000+ kèo cược thể thao tốt nhất thị trường sở hữu tỷ lệ thưởng cạnh tranh đang được 3 NPH Sportsbook cập nhật mỗi ngày tại slot365 là gì . Bạn có thể thử sức với 40+ bộ môn khác nhau như: Bóng đá, bóng rổ, bóng chuyền, khúc côn cầu, Boxing, võ tổng hợp MMA,… TONY03-11O
xn88 app có mục “Tin tức ngành” cập nhật xu hướng iGaming toàn cầu – giúp bạn nắm bắt sớm các tựa game hot sắp ra mắt tại Việt Nam. TONY05-15